Gastroparesis, EDS & the Final Piece of the Jigsaw Part #3 / Cranio-cervical Instability!
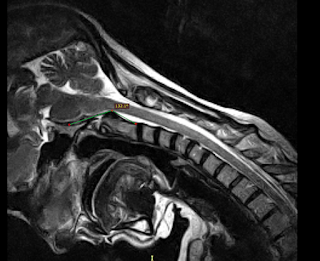
I know I left Part 2 somewhat in the middle of the consultation, so I'll try and start where I left off and see where it goes. Obviously there are inevitably going to be more "parts" to this series the deeper we go, so bear with me I WILL get it all down on here eventually. To sum up the last post in a few words, the diagnostic term for my neck issues is, Cranio-Cervical Instability. Naturally our next question was, "What can we do about it and what does it mean for the future?" This is where I struggle to explain. When it comes to brain/spinal surgery the decision process is not so cut and dry! So, the only way to actually fix the instability in my head and neck and prevent any further neurological damage would be to fuse my skull and top two vertebrae together using metal rods (permanently immobilising my skull C1 & C2) and remove the excess tissue that is causing the brainstem compression. Obviously this is a very risky procedure and not one...